Accessing insurance coverage for durable medical equipment is critical to making ALS livable for everyone, everywhere, until we find a cure. However, too many private insurers either refuse to cover or set up insurmountable barriers for patients who desperately need access to the equipment they need to survive.
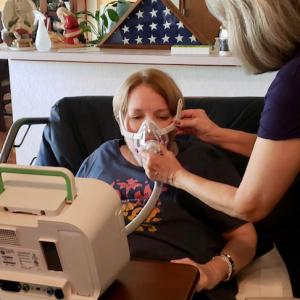
In the case of noninvasive ventilators, this could mean insurers force someone living with ALS to try a lower-cost ventilation machine and prove that it is not working before gaining access to the equipment they truly need.
Physicians caring for people with ALS are in the best position to determine the course of care and the type of respirator needed, not insurers’ authorization and utilization staff. People living with ALS deserve the full benefit of their doctor’s experience and expertise, especially where it is focused on supporting their ability to breathe.
But don’t take our word for it, learn from people living with ALS and their families around the country who are facing these difficult challenges every day.
Andrew, Denver, CO: Age 62, Diagnosed with ALS in 2021
I have Medicare and Medigap Plan G insurance. I am at the point where a non-invasive ventilator is going to be an option. My doctor at National Jewish in Denver says I must make a decision on whether or not I want to do that or tracheotomy or hospice, no other choices. This wasn't part of my plan, getting ALS, it's not part of anyone's plan. However, my choice is to live on a ventilator or succumb to the disease and die in the next couple of months, if that is a choice. Having to battle insurance is not another battle I have the energy for. Does it really have to be this difficult?
Jacob, Winfield, WV: Age 24, Diagnosed with ALS in 2022

My name is Jacob Harper. I am a 24-year-old male from Winfield, WV. I am told I am the youngest person in WV living with this dreadful disease. I was diagnosed with a nano-rare, super aggressive, genetic version of ALS on March 9th, 2022. My doctor at Marshall Neurology prescribed a Trilogy ventilator for me last August 2022. My insurance company denied the device over and over for a period of six months. Multiple calls and video conferences were held by my doctor and his staff in an attempt to get the device approved. Finally, my father had to intervene and contact the insurance company directly. In February 2023, the company approved the Astral vent, not the Trilogy, as prescribed. The Astral is doing the job, but with a 1 – 3 year life expectancy, six months is an unacceptable waiting period.
Mary, Wadsworth, IL: Wife and Caregiver to Her Husband with ALS
Hello, my name is Mary and my husband had ALS and was on a noninvasive ventilator. He could not be off the ventilator for more than one minute due to the inability to breathe. We originally did not have any issues with the insurance company covering my husband’s ventilator, however my employer changed insurance companies to a different carrier, and they denied his coverage for the ventilator and suggested he use a less expensive device such as for sleep apnea. After numerous appeals by the physician, they still denied the coverage. Insurance companies should not dictate what a patient needs over what their physician orders. I explained to the insurance company my husband would die without this ventilator and that he needed it to breathe. This only fell on deaf ears at the insurance company; they were only looking at how they could save money. Insurance companies do not have the right to play God with patients’ lives.
Jade, Seattle, WA: Age 32, Daughter and Caregiver for her Mother Peggy
My mother had ALS for 3 years, she was diagnosed in 2018. She began having problems with breathing after only a year of her diagnosis. My mother didn't want any invasive measures to be taken, no feeding tube, no invasive ventilation. Having access to a noninvasive ventilator gave my mom the ability to be present and be with us for longer than she would have otherwise. She used multiple types of breathing machines, one attached to her wheelchair with a straw at mouth level for air, one with nose pillows if she was feeling really weak or breathless. Then, when she slept, she was on a Co2 bypass breathing machine with a mouth and nasal seal to keep her breathing through the night.
My mom suffered from severe claustrophobia and couldn't have a mask strapped to her face all day, the nasal pillows and breathing straw were imperative for her comfort and her survival. It makes me sad and angry to think that people dying from ALS would need to fight insurance and Medicare on getting access to these life saving devices. ALS is one of the hardest things to watch a person die from, let alone having to fight for their breath.
Mary, Saint Paul, MN: Wife and Caregiver to her Husband Tom
My name is Mary. I am relating my husband Tom's experience. We live in Saint Paul, MN. Tom was 69 when he was diagnosed with ALS in October 2019. The results from his first pulmonary function test in November 2019 indicated his need for a BiPap. It was denied by his Medicare Advantage insurer. His ALS clinic physician wrote a letter of appeal but the coverage for the device was denied again. The doctor continued to advocate for him with the insurer.
After a December weekend with Tom taking frequent long naps, our daughter did research and contacted the ALS clinic to ask if we could purchase a similar device until we could get insurance coverage for a BiPap. We planned to switch insurers for the next year. Her inquiry reached Tom's doctor who called me concerned that he needed immediate intervention. On December 23, 2019, we went to the emergency room.
Per the attendant, his blood CO2 level would kill most people. He spent the night at the hospital on a BiPap, his doctor contacted The ALS Association chapter for a machine from their equipment loan pool and Tom was discharged at noon on Christmas Eve. At 5:00 the respiratory tech brought the machine, showed us how to use it and wished us a “Merry Christmas.”
A nurse from the insurance company called when the bills were received, and I explained the situation. We were charged for the emergency room copay and one of the blood tests. We never saw any other bills; I assume because the insurance company realized they were at fault for Tom's hospitalization. The BiPap kept Tom alive until September 2021. We are eternally grateful to the medical team, The ALS Association and the durable equipment provider for their care and concern for those 22 months.

This is just a handful of people we’ve heard from in the ALS community who are fighting for their right to breathe and live the life they choose. We are committed to empowering people with ALS and their families to advocate with private insurers and insurance regulators for policies that make sure durable medical equipment and ALS treatments are not only available, but accessible to all regardless of where they live.
Special thanks to all of our advocates who are sharing their stories to help fight for change for people living with ALS and their families. You can join them today by sharing your story HERE.
To learn more about how you can become and advocate and join the fight to help the ALS community, visit our website HERE.
To learn more about some of the work being done to break down barriers set by insurance companies, listen to our Connecting ALS podcast episode, “Making Insurance Accessible for People Living with ALS.”
To continue to follow stories about people living with ALS in the community and learn more about the disease, subscribe to receive our weekly blogs in your inbox HERE or follow us at als.org/blog.


Join the conversation. Please comment below.