For many people living with ALS, the decision to have a feeding tube placed, if or when it’s needed, is an important one, and as with many decisions that must be made during an ALS journey, it’s not of the one-size-fits-all variety. In recognition of Feeding Tube Awareness Week, we wanted to share some common concerns and misconceptions about them as well as some resources to help.
You shouldn’t have a feeding tube placed until you really need one.
While the right time to consider a feeding tube will vary depending on your individual circumstances, for a person with ALS, an unintended loss of 10 percent of body weight is usually a good indicator that a feeding tube may be beneficial. Other signs to be aware of are when eating leads to fatigue, when one has difficulty eating enough to sufficiently nourish themselves or when one has difficulties with chewing, gagging, or swallowing. Recognizing these challenges will allow you and your care team to be proactive in the decision-making process.
Getting a feeding tube is a painful process.
While it is true having a feeding tube placed is a surgical procedure, it is generally a safe, simple procedure that can take as little as 30 minutes. There are two ways to place the tube, either using an endoscope through the mouth to the stomach wall or under guidance of an x-ray machine. If there are no complications, the person often can go home the same day or at most after an overnight stay in the hospital. In most cases the procedure causes no more than mild pain and discomfort for a short period of time.

If I have a feeding tube, I cannot eat by mouth.
A feeding tube allows a person with ALS to meet fluid and nutrition needs without the difficulty and exhaustion of the eating process, but that does not mean you cannot eat by month if and when you want to. With the feeding tube providing the main source of getting the needed calories, eating and drinking by mouth can be saved for pleasure and enjoyment.
Feeding tubes are only for food.
While it is called a “feeding” tube, the name is a bit of a misnomer. In many cases, it can also be used to deliver medications as well. Some pills can be ground up and liquids can be delivered this way if swallowing becomes a problem, ensuring a person with ALS is getting enough hydration when drinking by mouth is a challenge. Consult with your care team to determine the safest options for you.
Once I have a feeding tube, I won’t be able to go out of the house without being hooked up to something.
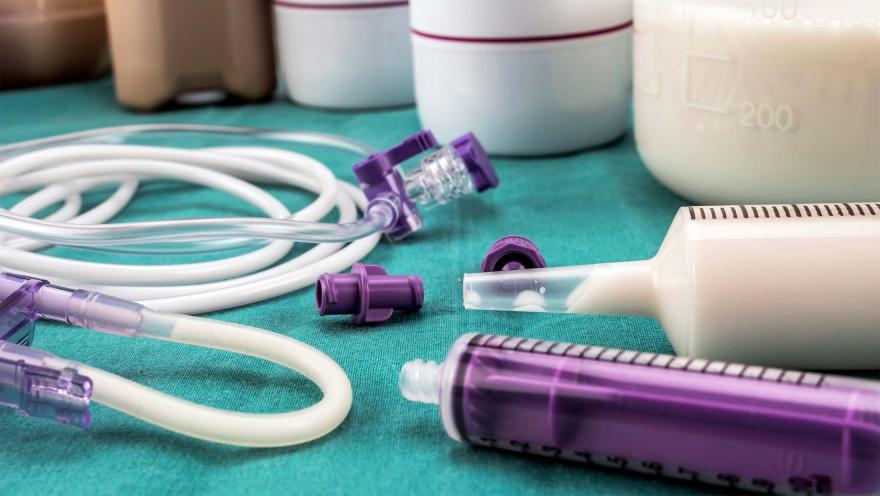
Once placed, the equipment needed to use the feeding tube is minimal and does not require much space to transport. With bolus feeding, all that’s needed is a syringe and formula. In cases where there are severe digestive issues, a pump may be necessary, but in all likelihood a person with ALS who chooses to have a feeding tube placed will see minimal impact on their ability to leave the house, socialize, and do other things they enjoy.
Ultimately, the decision to have a feeding tube placed is a personal choice for a person with ALS and their caregivers. It is important to plan ahead and discuss the different options with your care team to help weigh the pros and cons and understand how the decision will affect your overall quality of life.
The following resources have been developed to provide you with the knowledge you need to help make this decision with the minimum amount of stress and difficulty.
- ALS.org: Nutrition & Feeding Tubes
- ALS Association Resources Guide: Adjusting to Swallowing Changes and Nutritional Management in ALS
- Webinar: Promoting Adequate Nutrition - How a Feeding Tube Helps
- ALS Association Factsheet: FYI: Information About Feeding Tubes
- ALS.org Blog: What to Know About Feeding Tubes and Decision Making When Living with ALS
- Connecting ALS Podcast: "Feeding tubes and the Mind Body Connection"
To continue to follow stories about people living with ALS in the community and learn more about the disease, subscribe to receive our weekly blogs in your inbox HERE or follow us at als.org/blog.

Comments
I feel a bit more at ease about the use of a feeding tube.
My wife has ALS. She is now in her 6th week of hospice care. She is on a feeding tube for nutrition and medications. She is ready for this to end and she wants to discontinue the feeding tube. She cannot speak, confined to a power chair, cannot use legs or hands at all. Basically, she is like a 140 lb. baby with a feeding tube. If she discontinues the feeding tube, will this be considered suicide. She was diagnosed with ALS in May of 2019.
Frank, my heart goes out to you and your wife. So sorry.
I just had feeding tube installed because I no longer can swallow.
Previous throat cancer and radiation in 1997.
I have both my lower jawbone placed , left side 2002 and right side 2012.
Since then I had to blend my food like a real thin smoothie, however lately that is no longer working.
I got covid19 and plus I have pneumonia. I went from weighing 150 lbs
6 months to 120 lbs currently.
I in a rehab center to regain my weight and strength.
I will start my rehab 12/26/2023. I do have good care.
I am looking a device to shutdown and open the tube.
“… for a person with ALS, an unintended loss of 10 percent of body weight is usually a good indicator that a feeding tube may be beneficial.”
I can still chew and swallow just fine. But I’ve gone from 216 lbs to 129 lbs so way more than 10% weight loss.
What this article does not mention is care of feeding tube on top of everything else a caregiver has to do, which is considerable.
I’ll probably get one soon but I’m tired of making concessions to this infernal disease.
Join the conversation. Please comment below.